Resubmitting a Medicare or DVA claim
Only failed, lost, or delayed bulk bill or DVA claims can be resubmitted. Patient Claims that are stuck in a “With Medicare” state need to be reviewed with Medicare by the Client. They can be resubmitted using the
manual decline option.
How to resubmit a claim
Open the Medicare Claim History report from Reports > Medicare
Select the relevant time period and click Get Data
Select the Failed tab
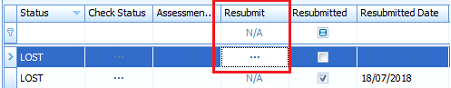
Find an item to be resubmitted and click the button in the Resubmit column.
This action:
-
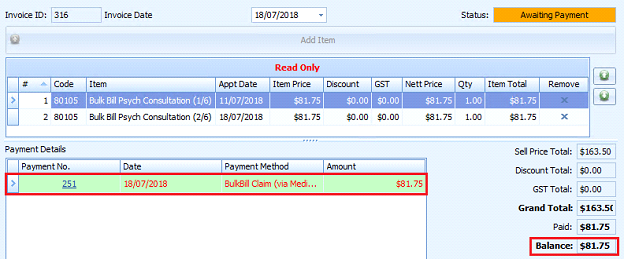
Opens the relevant invoice in Invoices
-
Zeroes the current payment against the invoice
OR
-
If there is more than one item on the Invoice, it adjusts the payment balance to the amount paid
The text payment line will turn RED
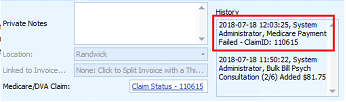
A note will be added to the Invoice History to record the change.
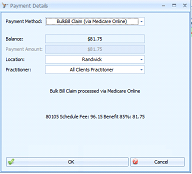
In the Invoice, click Add Payment.
Only the balance due to be paid will display in the Payment Amount
Click OK
Continue to process the payment or claim in the usual way.
If a payment type of BB or DVA claim is selected:
-
Only the unpaid BB or DVA Item will be resubmitted. In the Medicare Claim History Report, the
Resubmitted check box is ticked and the
Resubmitted Date added for the original claim.
-
There is a link in the Claim History Report in the
Link to Record field to the original claim.
-
Th
e Claim Number is updated on the Invoice to the new Claim Number.
If another type of payment is selected, this will be processed as normal:
-
No changes are made in the
Medicare Claim History Report -
It
may be prudent to enter a note against the original claim to acknowledge that payment has been taken in another manner.
Note: If Payment has been received via a manual BB or DVA process, then a Payment type of Manual BB or DVA claim could be added to track these if necessary.
What if the original invoice and or claim is no longer valid?
At this point there is only a workaround to deal with this. A process to manage these is being developed.
This can be carried out as follows:
1. Carry out the first part of the resubmission as above but do not add a Payment.
2. Update the Item Price in the Invoice Line item to $0.00
3. Click Save
Adding a note both in the Invoice Private Notes and Medicare Claim History Report notes will be useful in ensuring the transparency of this process.